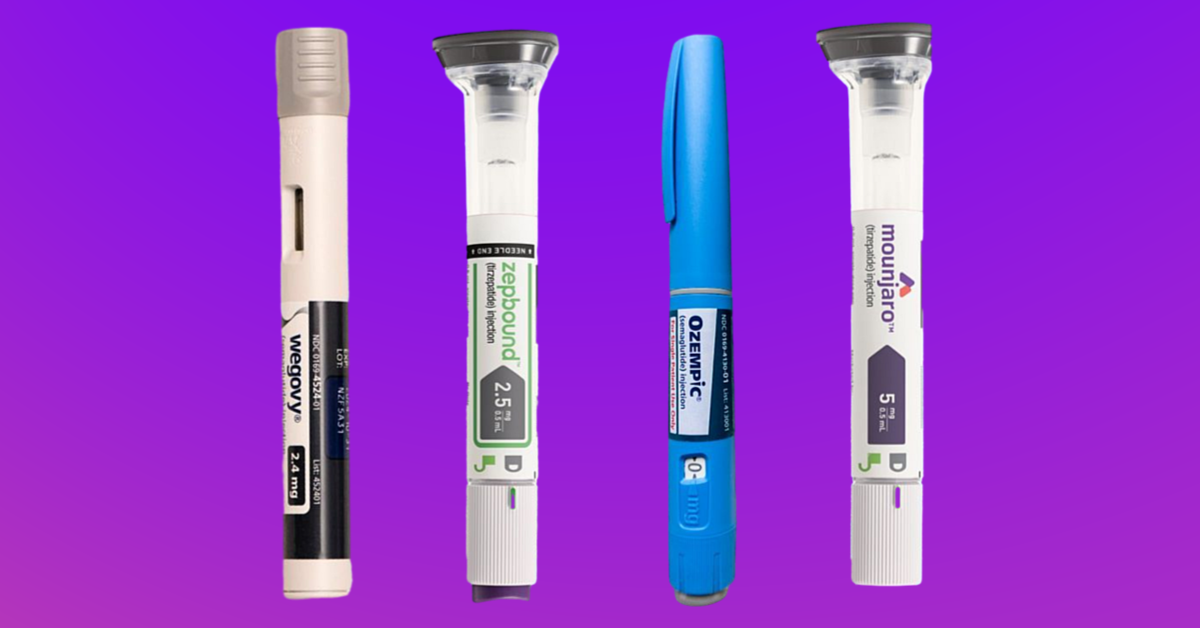
Injectable weight loss medications have rapidly moved from niche therapies to major players in both obesity and type 2 diabetes (T2D) care. Drugs like semaglutide, tirzepatide, and newer experimental triple agonists deliver levels of weight loss that were previously seen only with bariatric surgery, while also improving blood sugar and cardiovascular risk.
Rising Interest in Injectable Weight Loss Drugs
Obesity and T2D are tightly linked through insulin resistance, inflammation, and excess visceral fat, so targeting weight has become a central strategy in diabetes management rather than a secondary goal. Modern incretin‑based injectables are designed to support long‑term, clinically meaningful weight loss while addressing core metabolic dysfunction.
This article walks through how these drugs work, what the latest trials show, safety considerations, how guidelines use them, and practical questions to discuss with your healthcare team.
How Modern Injectable Weight Loss Drugs Work
Incretin Hormones and Appetite Regulation
Incretins are gut hormones released after meals that help regulate blood sugar and appetite. Two key incretins, GLP‑1 (glucagon‑like peptide‑1) and GIP (glucose‑dependent insulinotropic polypeptide), increase insulin in a glucose‑dependent way, suppress glucagon, slow stomach emptying, and act on the brain to reduce hunger.
GLP‑1 Receptor Agonists
GLP‑1 receptor agonists (GLP‑1 RAs) are injectable drugs that mimic the effects of natural GLP‑1. By activating the GLP‑1 receptor, they lower blood glucose, promote early satiety, and reduce food intake, leading to significant weight loss in many patients.
Dual GIP/GLP‑1 Agonism: Tirzepatide
Tirzepatide is a once‑weekly injectable that activates both the GIP and GLP‑1 receptors, providing a dual incretin effect. This dual action appears to drive greater weight loss and stronger glucose lowering than traditional GLP‑1–only drugs in clinical trials.
Triple Agonism: Retatrutide
Retatrutide is an investigational “triple agonist” that targets receptors for GLP‑1, GIP, and glucagon, aiming to combine appetite suppression with increased energy expenditure. Early trials suggest that adding glucagon receptor activity may further increase fat loss and improve metabolic health compared with single or dual hormone approaches.
Current GLP‑1 Receptor Agonists for Weight Loss and Diabetes
Key Agents: Semaglutide and Liraglutide
Semaglutide and liraglutide are among the most widely used GLP‑1 RAs for both T2D and chronic weight management. Semaglutide is available as Ozempic for diabetes and Wegovy for obesity, while liraglutide is available as Victoza for diabetes and Saxenda for weight management in many markets.
Weight‑Loss Efficacy of Semaglutide
In major obesity trials and subsequent real‑world data, higher‑dose semaglutide for weight management has produced average weight loss of around 10–15% of initial body weight in many participants. These results represent a major advance over older medications, which typically led to modest weight loss of only a few percent.
Glycemic and Cardiometabolic Benefits
In people with T2D, semaglutide often reduces A1c by roughly 1–1.5 percentage points, while also improving blood pressure, lipids, and markers of insulin resistance. Large cardiovascular outcome trials have shown that GLP‑1 RAs can lower the risk of major adverse cardiovascular events in high‑risk patients.
Role in Current Guidelines
Recent diabetes guidelines recommend GLP‑1 RAs as prioritized options for people with T2D and obesity, especially those with cardiovascular disease or chronic kidney disease. These agents are increasingly used earlier in treatment to address both glucose and weight, rather than being added late after insulin.
Tirzepatide: Dual GIP/GLP‑1 Agonist for Diabetes and Obesity
Mechanism and Approvals
Tirzepatide is approved for T2D and obesity under different brand names depending on the region. By activating both GIP and GLP‑1 receptors, it enhances insulin release, suppresses appetite, and improves multiple aspects of metabolic health.
Weight‑Loss Outcomes in People Without Diabetes
In large obesity trials in people without diabetes, tirzepatide has produced average weight loss around 20% of initial body weight, with some participants approaching 25% loss over longer treatment. Head‑to‑head data suggest tirzepatide may lead to greater weight loss than semaglutide at obesity doses.
Glycemic Control in Type 2 Diabetes
Across multiple phase 3 trials in T2D, tirzepatide has lowered A1c by up to about 2 percentage points and produced greater weight loss than semaglutide 1 mg or basal insulin. This positions tirzepatide as one of the most potent injectable options for both glucose lowering and weight reduction in diabetes.
Real‑World Data and Broader Metabolic Effects
Real‑world analyses have found that average weight loss at one year with tirzepatide is higher than with semaglutide, although patient populations and dosing can differ. Tirzepatide is also being studied, and in some regions approved, for conditions like obstructive sleep apnea and fatty liver disease, reflecting its broader metabolic impact.
Guideline Positioning
Updated guidelines place tirzepatide alongside GLP‑1 RAs as a preferred option when weight loss is a major goal and as an alternative to intensifying insulin. For individuals with T2D and obesity, these agents are often prioritized over older therapies that do not promote weight loss and may cause weight gain.
Emerging Triple Agonists: Retatrutide and Beyond
What Is Retatrutide?
Retatrutide is an investigational injectable that activates three receptors—GLP‑1, GIP, and glucagon—making it a “triple agonist.” It is under active study for obesity, T2D, and metabolic dysfunction–associated steatotic liver disease (MASLD).
Phase 2 Weight‑Loss Data in Obesity
In phase 2 obesity trials, higher doses of retatrutide have led to average weight loss in the range of about 23–24% at around one year in people with obesity but without diabetes. These results are comparable to or even greater than the best outcomes seen with current GLP‑1 or dual agonists, though they come from earlier‑stage research.
Results in Type 2 Diabetes
In participants with T2D and obesity, retatrutide has shown roughly mid‑teens percentage weight loss at several months, along with substantial improvements in blood glucose. These findings suggest that triple agonists could become powerful tools in diabetes and obesity management if longer‑term safety and efficacy are confirmed.
Metabolic and Organ‑Level Effects
Early trials report reductions in visceral fat, liver fat, and improvements in insulin sensitivity and lipid profiles with retatrutide. These broader effects are particularly relevant for people with fatty liver disease and high cardiometabolic risk.
Future Directions for Triple Agonism
Researchers view triple agonists as the next generation after GLP‑1 and dual GIP/GLP‑1 agonists, aiming for greater efficacy with manageable side effects. However, long‑term safety data, cardiovascular outcome trials, and regulatory decisions are still in progress.
Safety, Side Effects, and Long‑Term Considerations
Typical Side Effects Across These Drugs
GLP‑1 RAs, tirzepatide, and emerging triple agonists share many gastrointestinal side effects, including nausea, vomiting, diarrhea, constipation, and early fullness. These symptoms are usually most intense during dose escalation, and slower titration plus smaller, lower‑fat meals can improve tolerability.
Serious but Less Common Risks
Less common but important risks include pancreatitis, gallbladder disease, and rare bowel complications such as ileus or intestinal obstruction. Patients with prior pancreatitis, gallstones, or certain gastrointestinal conditions may need closer monitoring or alternative therapies.
Drug‑Specific Safety Notes
Some analyses suggest tirzepatide may carry a higher relative risk of vomiting compared with certain GLP‑1 RAs, though the overall safety profile remains acceptable in clinical trials. Early data indicate that retatrutide’s gastrointestinal side effects are broadly similar to existing incretin‑based therapies, but follow‑up is still limited.
What Happens When Treatment Stops?
When GLP‑1 or GIP/GLP‑1 therapy is discontinued, many patients experience partial or substantial weight regain over time. For this reason, experts increasingly consider these drugs as chronic, long‑term treatments, similar to medications for blood pressure or cholesterol.
Knowledge Gaps and Ongoing Trials
Key open questions include the long‑term safety of very high and prolonged doses, effects on cardiovascular and kidney outcomes for newer agents, and any potential cancer signals. Ongoing and planned outcome trials will help clarify these issues over the next several years.
How Guidelines Now Use These Drugs in Diabetes Care
From Glucose‑Only to Weight‑Centric Management
Recent standards of care emphasize weight, cardiovascular risk, and kidney protection as primary goals alongside glucose control. This shift reflects evidence that weight‑loss medications can significantly impact long‑term outcomes, not just numbers on the scale.
Recommendations for Obesity
For people with obesity, particularly when T2D or high cardiometabolic risk is present, guidelines recommend GLP‑1 RAs and tirzepatide as preferred pharmacotherapies. These agents are intended to be used in conjunction with lifestyle interventions rather than as stand‑alone solutions.
Position in Type 2 Diabetes Treatment Algorithms
GLP‑1 RAs and GIP/GLP‑1 agonists are now preferred options for intensifying therapy in T2D, often before starting or escalating insulin, especially in people with obesity, cardiovascular disease, chronic kidney disease, or heart failure with preserved ejection fraction. This reflects their dual benefits on glycemia and weight, as well as cardiovascular and kidney outcomes.
Combining With Other Agents
Guidelines support combining GLP‑1 or GIP/GLP‑1 agonists with SGLT2 inhibitors and other cardioprotective drugs to create comprehensive regimens that target multiple pathways. Such combinations may provide additive benefits on weight, blood pressure, kidney function, and heart failure risk.
Practical Considerations for Patients and Clinicians
Who Might Benefit Most?
These injectable therapies may be especially beneficial for people with T2D and obesity, those with high cardiovascular or kidney risk, individuals with obesity‑related complications like sleep apnea, and some with severe obesity but no diabetes. Eligibility depends on local approvals, BMI thresholds, comorbidities, and payer criteria.
Key Questions to Ask Your Healthcare Provider
Important questions include which drug is appropriate, expected ranges of weight loss and A1c change, how long therapy might continue, how to manage side effects, and how treatment fits into your broader health plan. Discussing other medications, medical history, and personal goals helps tailor the choice.
Integrating Lifestyle and Behavioral Strategies
Even with powerful medications, nutrition, physical activity, sleep, stress management, and psychological support are crucial for long‑term success. Lifestyle strategies can help preserve lean body mass, enhance metabolic improvements, and support weight maintenance if doses are reduced or stopped.
Access, Cost, and Insurance
Access to these drugs can be limited by cost and insurance policies, which may require specific BMI cut‑offs, documented comorbidities, or prior lifestyle attempts. Patients and clinicians often need to review coverage criteria, submit documentation, and consider assistance programs where available.
Looking Ahead: The Future of Injectable Metabolic Therapies
Pipeline Trends
The pipeline includes longer‑acting formulations, additional dual and triple agonists, and trials expanding into conditions like sleep apnea, liver disease, and cardiovascular prevention. Researchers are also exploring oral versions and combination therapies to simplify treatment and improve adherence.
Personalized Medicine in Obesity and Diabetes
As more agents become available, clinicians may be able to select drugs based on patient phenotype, comorbidities, genetics, and individual response. This personalized approach could optimize both efficacy and tolerability in managing obesity and diabetes.
Key Takeaways
Injectable incretin‑based therapies have transformed the landscape of obesity and diabetes treatment by combining meaningful weight loss with major metabolic and cardiovascular benefits. For many people, these medications can be powerful tools when used as part of a long‑term, whole‑person approach that includes lifestyle change and ongoing medical support.
###
Remember, proactive self-care matters. Every step we take, every decision we make to better manage our diabetes makes a difference in how well and how long we live. Choose wisely. Live long, love life and be well.
The information on this site is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. The information on this site is for informational purposes only and is not intended to diagnose, treat, or cure any type of disease or condition. Diabetes Control Today does not guarantee any results for your specific situation. In support of our website, we may share resources offered by trusted partners. If you purchase products from any of these partners, the owners of this site may receive a portion of the proceeds. These affiliations allow us to continue bringing you valuable, potentially life-changing content. Some content on this site has been generated by AI.