I understand that exhaustion. I know what it’s like to want to make a change but not know where to start, or to feel like the connection between what you do and what your blood sugar actually does is just… invisible. That invisibility is the hardest part. And that’s exactly why what I’m about to share feels so important to me — because a small device worn on your arm might finally be the thing that makes that connection visible.
Continuous Glucose Monitoring, or CGM, has long been associated with people using insulin — the sensors, the alerts, the data streams. But a growing body of clinical evidence, including a compelling 2025 case series published in Clinical Diabetes by the American Diabetes Association, is showing that CGM’s most powerful role may not be in insulin dosing at all. For people with type 2 diabetes who aren’t using insulin, CGM can function as something much more personal: a real-time behavior modification tool that turns abstract advice into immediate, personalized feedback.
The American Diabetes Association has long recommended lifestyle modification — specifically changes in food intake and physical activity — as the very first line of treatment for type 2 diabetes. This is sound, evidence-based advice. The challenge is that it’s also painfully vague when you’re standing in a grocery store aisle, or sitting down to dinner after a long day, with no way of knowing whether the choice you’re about to make will send your blood sugar soaring or keep it steady.
Sustaining meaningful behavioral change is notoriously difficult under the best of circumstances. Without immediate, personalized feedback, even highly motivated people struggle to connect their daily choices to their long-term outcomes. That’s not a willpower problem — it’s a feedback problem. We are wired, as humans, to respond to consequences that are immediate and visible. When consequences are delayed by months (like a quarterly A1C result), the behavioral signal is weak.
“We are wired to respond to consequences that are immediate and visible. A quarterly A1C test is a weak behavioral signal. A real-time glucose graph is not.”
What CGM Actually Does — and Why It’s Different
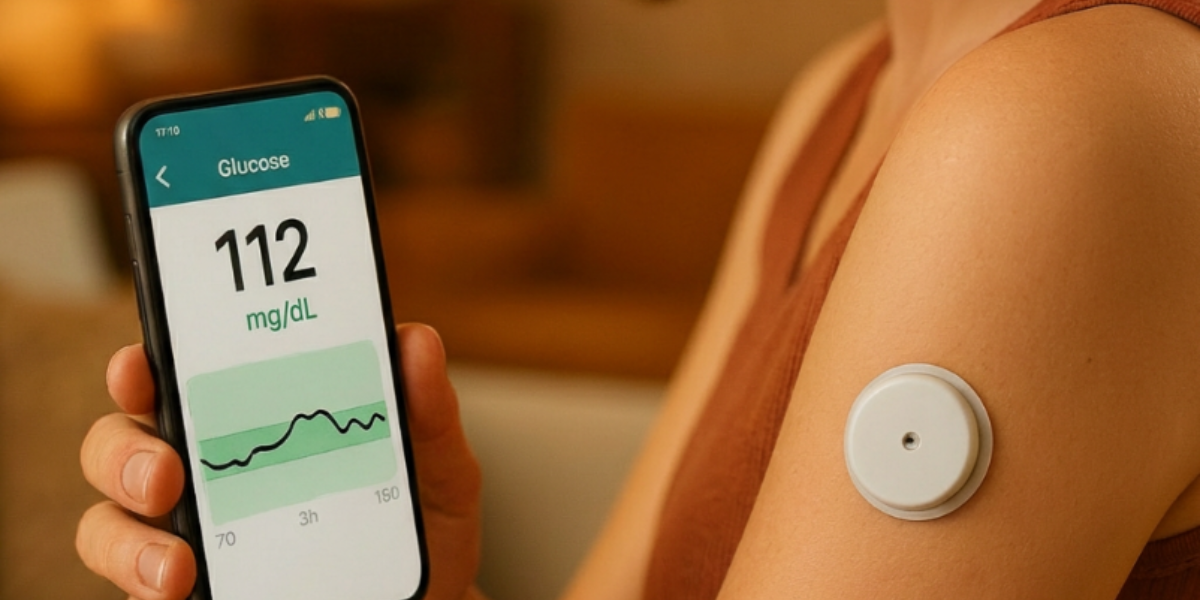
A CGM system is a small sensor, typically worn on the back of the arm or abdomen, that measures glucose levels continuously throughout the day — every few minutes — rather than just when you prick your finger. This data streams to a phone or reader, giving you a living, breathing picture of how your blood sugar rises and falls in response to what you eat, how you move, how you sleep, and even how stressed you are.
There are two main types. Real-time CGM (rtCGM) delivers continuous readings and alerts automatically. Intermittently scanned CGM (isCGM) requires the user to wave a reader or phone over the sensor to get a reading, but still captures data continuously in the background. Both can be profoundly illuminating — especially for someone who has never seen their glucose story told in anything other than a single number at a single moment in time.
The AGP Report: Your Glucose Story at a GlanceOne of the most clinically useful outputs from a CGM is the Ambulatory Glucose Profile (AGP) — a standardized report that compresses days or weeks of glucose data into a single, readable graph. It shows your median glucose curve, variability bands, the percentage of time you spend in your target range, above it, or below it.
Researchers and clinicians involved in the 2025 Clinical Diabetes case series found that reviewing the AGP collaboratively — patient and dietitian or diabetes educator together — significantly deepened insight and motivation. Seeing patterns laid out visually, like a predictable post-dinner spike or a mid-morning crash, makes abstract advice feel concrete and actionable.
A Real Example: From 20% to Meaningful Progress
Patient Profile: 38-Year-Old Man, Type 2 Diabetes
In one of the cases described in the Clinical Diabetes paper, a 38-year-old man with a five-year history of type 2 diabetes was managing his condition with metformin alone. Before starting CGM, his numbers told a difficult story.
After switching to a personal, real-time CGM paired with nutrition education sessions with a registered dietitian nutritionist (RDN) and certified diabetes care and education specialist (CDCES), the patient began to see — in real time — how specific foods and behaviors moved his glucose. The CGM closed the loop between behavior and consequence in a way that no amount of well-intentioned advice had managed to do before.
The Science Behind the Behavior Change
Why does seeing your glucose in real time work when verbal advice often doesn’t? The mechanism is rooted in basic behavioral psychology: biofeedback. When we can observe the direct, immediate effect of our actions, we are far more capable of modifying those actions. CGM transforms nutrition education from something abstract and forward-looking into something immediate and personal.
Eat a bowl of white rice and watch your glucose spike to 220 mg/dL within 45 minutes? That image stays with you in a way that a dietitian saying “refined carbohydrates raise blood sugar” simply cannot. Eat a chicken and vegetable stir-fry over cauliflower rice and watch that same post-meal window stay flat? That’s a reinforcing reward that motivates the next good choice.
This is exactly the approach described by Ettestad and colleagues in the 2025 case series. The clinical team — comprising registered dietitian nutritionists and certified diabetes care and education specialists working alongside physicians — used CGM not just as a measuring tool but as a teaching and motivating tool. The AGP report became a conversation starter, a way to connect the dots between specific foods, meals, timing, and glucose outcomes in a language the patient could understand immediately.
What Gets Reinforced
The ADA’s Standards of Care already recommend specific evidence-based nutrition strategies for people with type 2 diabetes: increasing whole foods and nonstarchy vegetables, and reducing refined carbohydrates and ultra-processed foods. CGM data makes these recommendations tangible. When a patient can see the glycemic difference between a piece of fruit eaten alongside protein versus eaten alone, the guideline becomes a lived insight rather than a dietary rule handed down from on high.
A Landmark Shift: Starting WithThe 2025 ADA Guidelines
It’s worth pausing on just how significant a moment 2025 was in the clinical recognition of CGM for type 2 diabetes. For years, CGM recommendations were largely restricted to people using insulin or at significant risk of hypoglycemia — situations where the moment-to-moment data had clear, urgent clinical utility. Non-insulin users were largely left out of the conversation, and insurance coverage reflected that.
In 2025, the American Diabetes Association added a new recommendation: consider CGM use for adults with type 2 diabetes using any glucose-lowering medication. This represented a meaningful evolution in how the medical community thinks about CGM — not just as a safety device, but as a tool for engagement, education, and behavior change.
Over-the-Counter CGM: A New AvenueThe 2025 guidelines also acknowledged over-the-counter CGM options — devices that cost less than $100 per month and don’t require a prescription — as appropriate for people with type 2 diabetes not on insulin. The ADA notes that OTC CGM is specifically intended to provide behavioral insights related to diet and exercise, not to manage day-to-day insulin dosing. Using one for a few two-week periods per year may be both clinically useful and more affordable than continuous use.
How to Make the Most of CGM as a Behavior Tool
Simply wearing a CGM sensor doesn’t automatically produce behavior change — the data has to be understood, contextualized, and acted upon. Here’s what the research and clinical experience suggests makes the biggest difference:
- Review data with a dietitian or diabetes educator. The 2025 case series authors emphasized that collaborative review of AGP reports with an RDN or CDCES significantly enhanced patient insight. Don’t try to interpret everything alone — bring a clinical partner into the conversation.
- Look for patterns, not just peaks. A single high reading isn’t as meaningful as a consistently elevated post-lunch window. Train yourself to look at the shape of your day rather than reacting to individual numbers.
- Pair CGM with nutrition education. The CGM data is most powerful when you have a framework to interpret it. Understanding why protein slows glucose absorption, or why fiber matters, helps you make sense of what you’re seeing.
- Consider a blinded “baseline” period first. Some patients in the case series used a professional, blinded CGM (one they couldn’t see in real time) before switching to a personal device. This gave both patient and clinician an unbiased look at baseline patterns before any behavior change was introduced.
- Focus on Time in Range (TIR), not just A1C. TIR — the percentage of readings between 70 and 180 mg/dL — gives a richer, more dynamic picture of glycemic health than A1C alone. Even small improvements in TIR, like moving from 20% to 50%, are clinically meaningful.
- Use the Diabetes Plate Method as your meal anchor. The ADA’s plate method — half nonstarchy vegetables, a quarter lean protein, a quarter quality carbohydrates — gives a simple, structural framework that pairs naturally with what you observe on your CGM.
You Deserve to See the Full Picture
For too long, non-insulin-using people with type 2 diabetes were told to make changes without being given the tools to see whether those changes were working. CGM changes that equation. It moves the feedback loop from quarterly lab draws to real-time data — putting knowledge, and therefore power, directly in the hands of the person living with diabetes.
Is it a cure? No. Is it a substitute for medical care, medication, or the deeply human work of changing habits? Absolutely not. But as a complement to those things — as a window into your own metabolic story, one you can read in real time and discuss with a care team — it may be one of the most meaningful tools now available to people with type 2 diabetes who don’t use insulin.
If you’ve ever felt like you were flying blind, managing your diabetes on faith and quarterly labs alone — ask your doctor about CGM. The picture it paints might be exactly the one you’ve been waiting to see.
Talk to Your Care Team
CGM access is expanding. Many options are now available with a prescription, and over-the-counter devices are increasingly affordable. Ask your doctor, registered dietitian, or certified diabetes care and education specialist whether CGM could work for you.
Primary Source: Ettestad TM, Willis HJ, Johnson E, Green CR, Bergenstal RM. “Continuous Glucose Monitoring (CGM) as a Behavior Modification Tool: A Case Series on CGM-Guided Nutrition in People With Type 2 Diabetes Not Using Insulin.” Clinical Diabetes. October 2025; 43(4):610–617. doi.org/10.2337/cd24-0106
Additional Reference: American Diabetes Association Professional Practice Committee. Standards of Care in Diabetes — 2025. Diabetes Care. 2025;48(Supplement 1).
###
Remember, proactive self-care matters. Every step we take, every decision we make to better manage our diabetes makes a difference in how well and how long we live. Choose wisely. Live long, love life and be well.
The information on this site is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. The information on this site is for informational purposes only and is not intended to diagnose, treat, or cure any type of disease or condition. Diabetes Control Today does not guarantee any results for your specific situation. In support of our website, we may share resources offered by trusted partners. If you purchase products from any of these partners, the owners of this site may receive a portion of the proceeds. These affiliations allow us to continue bringing you valuable, potentially life-changing content. Some content on this site has been generated by AI.